Dry Needling
In the early nineties Christian Gröbli and Ricky Weissmann developed a systematic trigger point dry needling concept. That method has since been continually developed and taught by the DGSA. Dry needling is now an accepted successful technique that is used by practitioners worldwide in pain management, especially for muscle pain. Dry needling is mainly used to treat myofascial trigger points and the fascia. Dry needling is a safe treatment technique which requires comprehensive and professinal training with sound knowledge of anatomy and palpation skills. Complications can be safely avoided as long as the practitioner follows our safety guidelines and considers contraindications. Dry needling must be applied under strict hygienic conditions using only disposable sterile needles and a disinfectant to disinfect the needled area. Our ultimate goal in our dry needling courses is safe and complication-free dry needling. There are basically two different types of dry needling: Trigger Point Dry Needling (TDN) and superficial dry needling (SDN). The proper technique must always be chosen and adapted according to the patient and his complaints.
Forms of Dry Needling
Trigger Point Dry Needling (TDN)
In TDN, also called intramuscular stimulation (IMS), the needle is inserted directly into the trigger point or taut band. This triggers a local twitch response (LTR) The LTR is a short contraction of the taut band, which is perceived by many patients as a sensation of muscular release and as a sign that the right trigger point was needled. In addition, there is evidence to support the therapeutic value of the LTR in enhancing the release of fascia related adhesions, as well as to reduce inflammation around the trigger point. Furthermore, dry needling stimulates the oxygenation of the contracted muscle fibers and the fascia, reduces inflammation, improves blood circulation and thus sustainably reduces the local tension in the tissue with long lasting results.
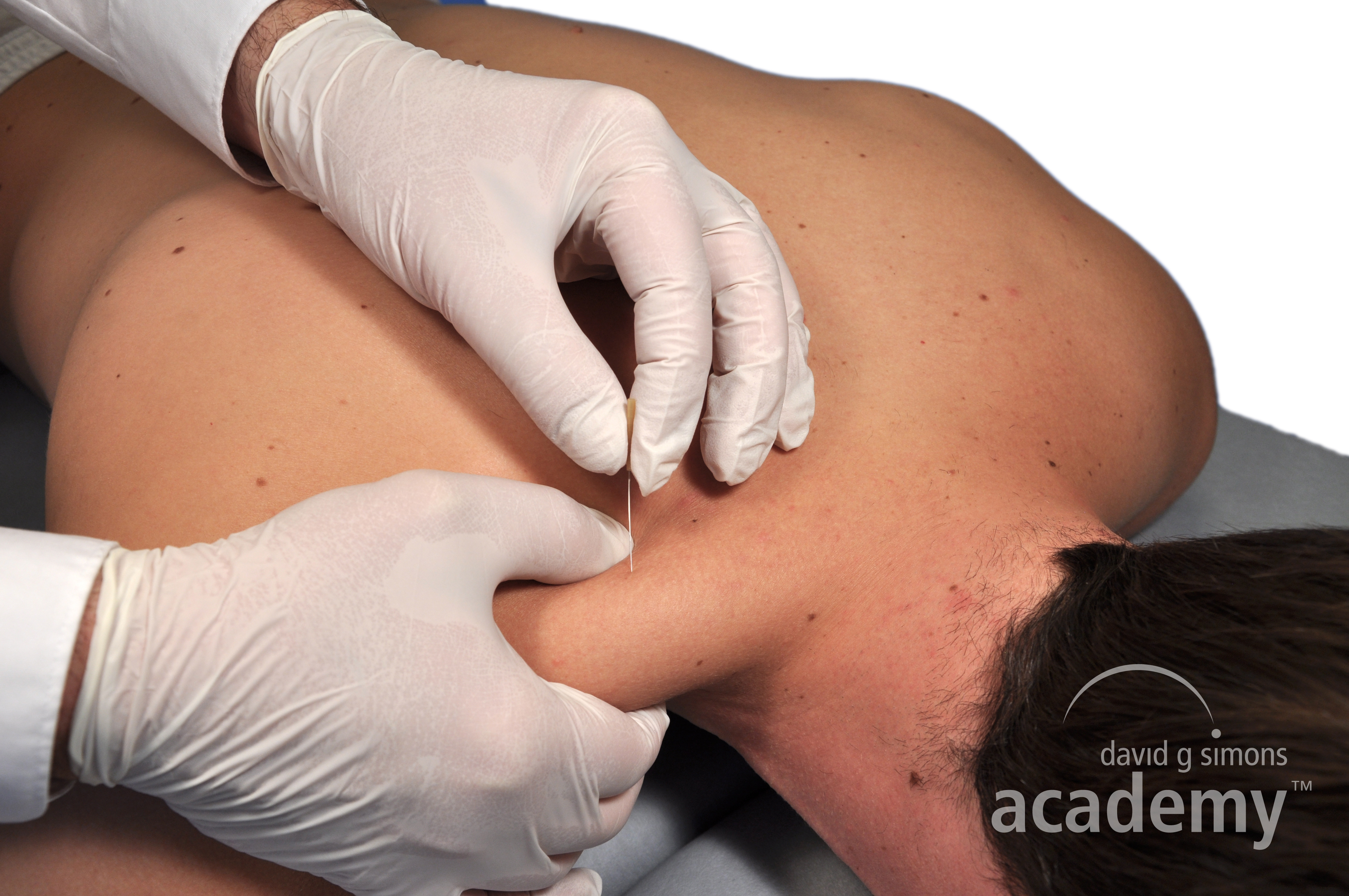
Superficial Dry Needling (SDN)
In superficial dry needling, SDN, the needle is inserted superficially obliquely to the skin surface, to about 3-4 mm above the trigger point or painful area. The effect of inserting a needle into the skin is manly to stimulate Aδ nerve fibers and thus activate inhibitory interneurons in the dorsal horn, leading to a gate control mechanism. The ratio behind the lasting effect on SDN for trigger points is, that the taut band relaxes due to the analgesic effect of the needling. In addition it has been shown that SDN can stretch connective tissue and activate fibroblast responses. After SDN, a palpable release of the taut band can be observed.
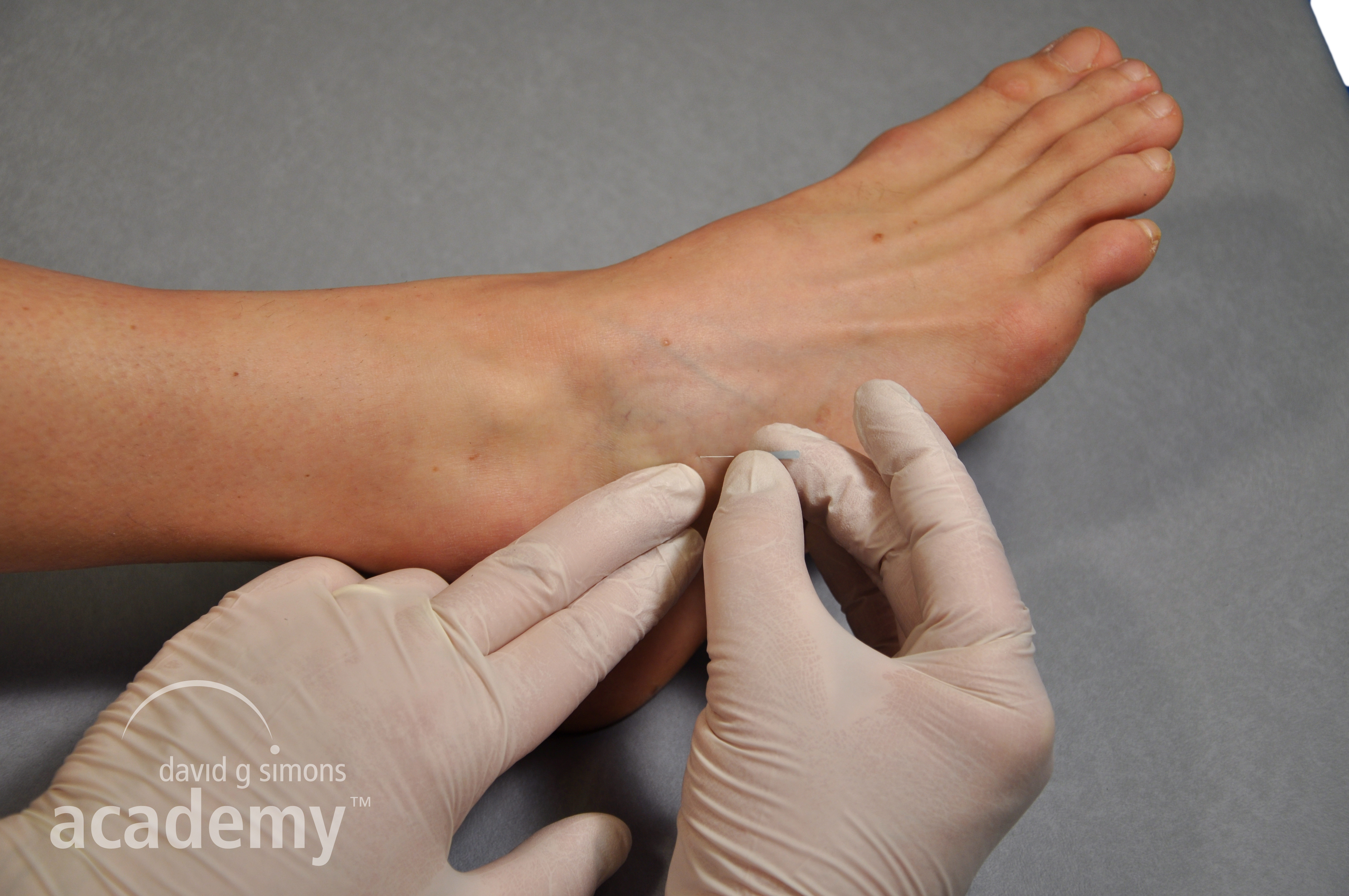
Intramuscular Electrical Stimulation (IMES)
Another method of dry needling is the intramuscular electrical stimulation (IMES), where at least two needles are inserted into the taut band and are stimulated by a 2-4 Hz-TENS currents. Due to the pulsating contractions of the taut band during electrical stimulation, it has a strong effect on the connective tissue mobilization. Patient often describe it like a deep massage. In addition, the 2-4 Hz-TENS current, induces an opioid mediated pain-relieving effect.
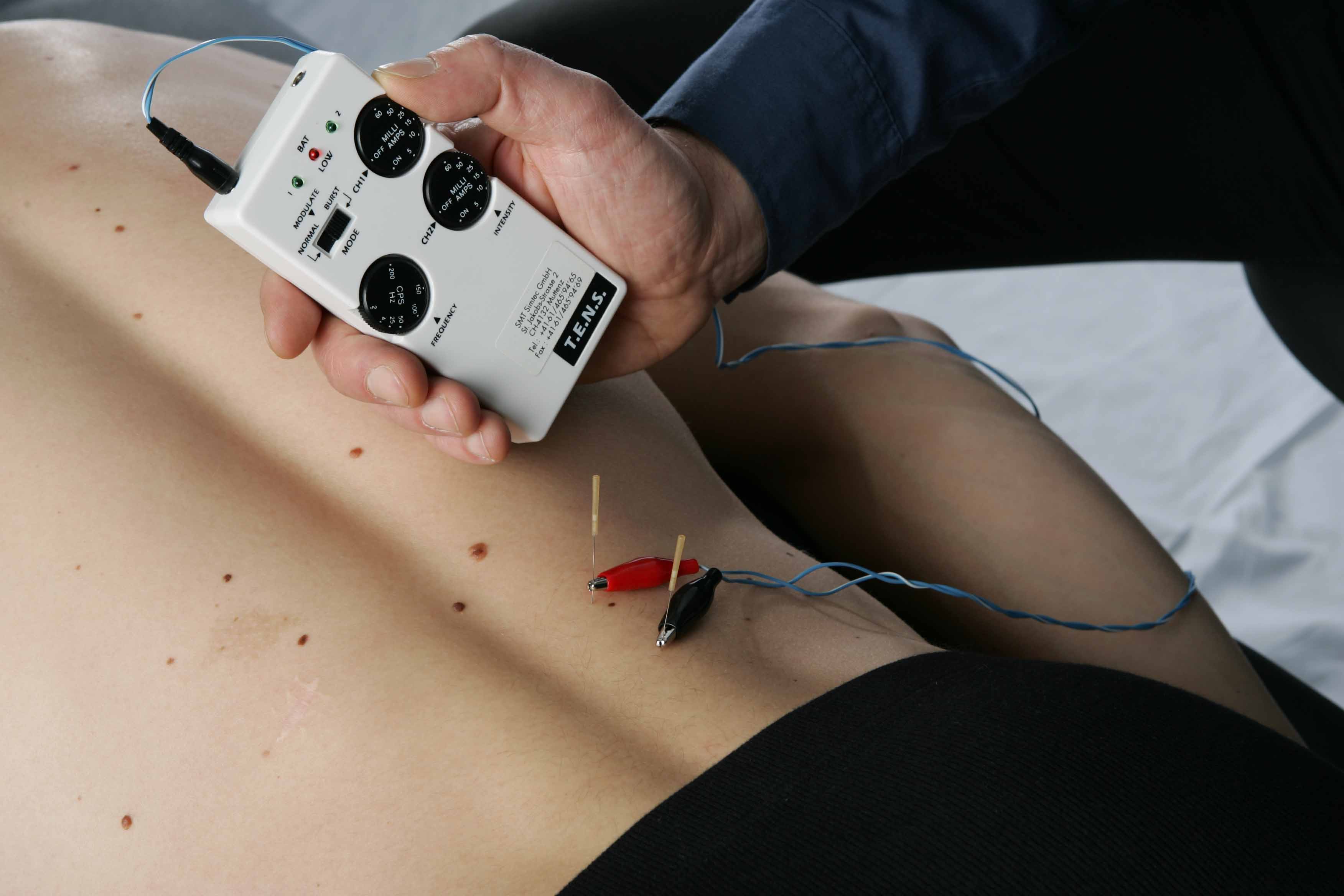
A Brief History of Dry Needling
Dry needling originated from clinical observations and studies treating trigger points using injections. Over time, evidence has shown that it was not the substance injected that was responsible for the release of the trigger point, but the accurate needling to the area. The work of Karel Lewit (1916-2014), a Czech doctor who published in 1979 the article "The Needle Effect in the relief of Myofascial Pain" in the renowned journal "Pain", as well as the work of Dr. P. Baldry and Dr. C. Gunn in the eighties, served as the benchmark for the development of the dry needling concept. In the early nineties Christian Gröbli and Ricky Weismann combined dry needling with Travell and Simons's findings of trigger point therapy and developed a systematic trigger point dry needling concept. That method has since been continually developed and taught by the DGSA. Dry needling is now an accepted successful technique that is used by practitioners worldwide in pain management.
